MD Curriculum

Medical students at NYU Grossman Long Island School of Medicine acquire knowledge in the basic and clinical sciences that underpin all medical practice while simultaneously gaining a fundamental understanding of health systems science—the study of how healthcare is delivered, how healthcare providers work together, and strategies to deliver safe, high-value patient care.
Our curriculum emphasizes integrated care—patient-centered care that delivers essential services to patients for clinical conditions across many medical disciplines—with effective communication and collaboration between community-based primary care providers and hospital-based specialists.
Students in our program earn a medical degree sooner and at reduced cost compared with students at other medical schools. Please view our academic calendars. Our graduates are prepared to transform healthcare delivery.
Phase One: Foundational Basic Science Instruction and Research
During Phase One, students spend 46 weeks engaged with interdisciplinary pre-clerkship coursework that covers foundational basic science concepts in biology, anatomy, and physiology. Students acquire skills in the behavioral and social aspects of practicing medicine that confer readiness to interact with patients and other healthcare providers during clerkship training in Phase Two.
The year begins with our Language Acquisition course, which integrates core basic science concepts with case-based clinical learning exercises. This course and subsequent organ systems courses are delivered in a dynamic mix of small and large group sessions that promote active learning.
There is one week of elective time, during which students choose an area of interest from a variety of primary care clinical topics.
The integrated longitudinal courses include core clinical skills training, with a focus on integrating communication skills with medical knowledge and clinical reasoning; health systems science education and foundational training in ethics, humanities, and professionalism; and exposure to ambulatory care practice.
Throughout Phase One, students participate in various learning modalities, including problem-based learning, small group seminars, large group lectures, workshops, clinical skills training sessions, clinical simulations, and bedside teaching.
Phase One Sample Schedule
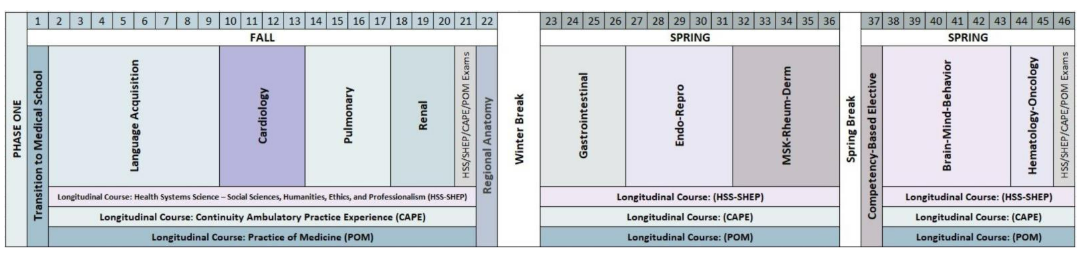
The schematic above represents our phase one schedule. All students progress through the first 46 instructional weeks of medical school on the same timeline. Students participate in longitudinal courses concurrently with organ systems courses.
During phase two, students spend 45 weeks in core clerkship training at NYU Langone Hospital—Long Island and our ambulatory care training sites. Throughout, students develop core clinical skills and consolidate medical knowledge to confer readiness for advanced training in phase three.
Students participate in core clerkships in internal medicine, neurology, obstetrics and gynecology, pediatrics, primary care, psychiatry, and surgery, as well as a core rotation in rehabilitation and pain management and two weeks of elective study.
Longitudinal courses meet once a week on a rotating schedule, including ambulatory care clinic, problem-based learning, health systems science, ethics and humanities, and radiology.
As a culmination of this phase, students take a comprehensive clinical skills exam, a series of simulated patient encounters that assess your skills in communication, taking patient histories, conducting physical examinations, and clinical reasoning.
Phase Two Sample Schedule
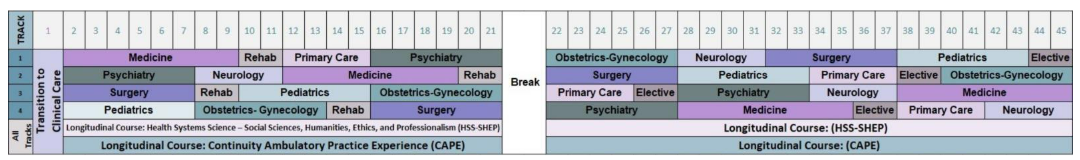
This schematic represents our Phase Two schedule. During this phase, students engage in a transition to clinical care orientation week and rotate through clerkship training in one of four schedule tracks over 45 weeks. The four different track schedules are depicted.
All students participate together in longitudinal courses in phase two, regardless of track.
Two-week electives are selected according to track schedules.
Phase Three: Advanced Skill Development, Individualized Exploration, and Career Preparation
Phase Three begins with a four-week structured independent learning course to prepare for the U.S. Medical Licensing Examination (USMLE) Step 1 examination and a three-week structured independent learning course to prepare for the USMLE Step 2 examination. Then, students spend 35 weeks completing longitudinal educational experiences, including a capstone project for HSS-SHEP. In addition to a clinical rotation in the emergency room and a critical care medicine (ICU) rotation, each student completes a sub-internship, or advanced clerkship, in either internal medicine, pediatrics, obstetrics and gynecology, or surgery. There are 12 weeks of elective time. Phase Three culminates in a transition to residency course.
Phase Three Sample Schedule
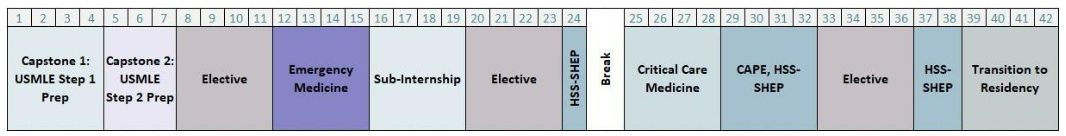
This schematic is an example of a Phase Three schedule; schedules vary. Students complete two structured courses to prepare for the USMLE Step 1 and Step 2 exams, a 4-week clerkship in emergency medicine, a 4-week ICU rotation, a 4-week subinternship (advanced clerkship), 12 weeks of electives, and a 4-week transition to residency course.