
Internal Medicine Residency Curriculum
NYU Grossman Long Island School of Medicine’s Internal Medicine Residency trains Internal Medicine physicians to provide the highest level of care to their patients and pursue a career in the setting of their choosing. With 66 categorical residents and 16 prelim residents annually, our internal medicine residents play an essential role in our health care system. They provide compassionate evidence based medical care for a wide spectrum of patients, providing care for all adult patients and for conditions that range from acute illnesses and urgent care health needs to continuity care for chronic disease management, prevention, and wellness.
We offer two tracks: a categorical medicine residency and a preliminary medicine residency track. The categorical medicine track is a three-year program that provides training in inpatient and ambulatory care for patients with medically complex conditions.
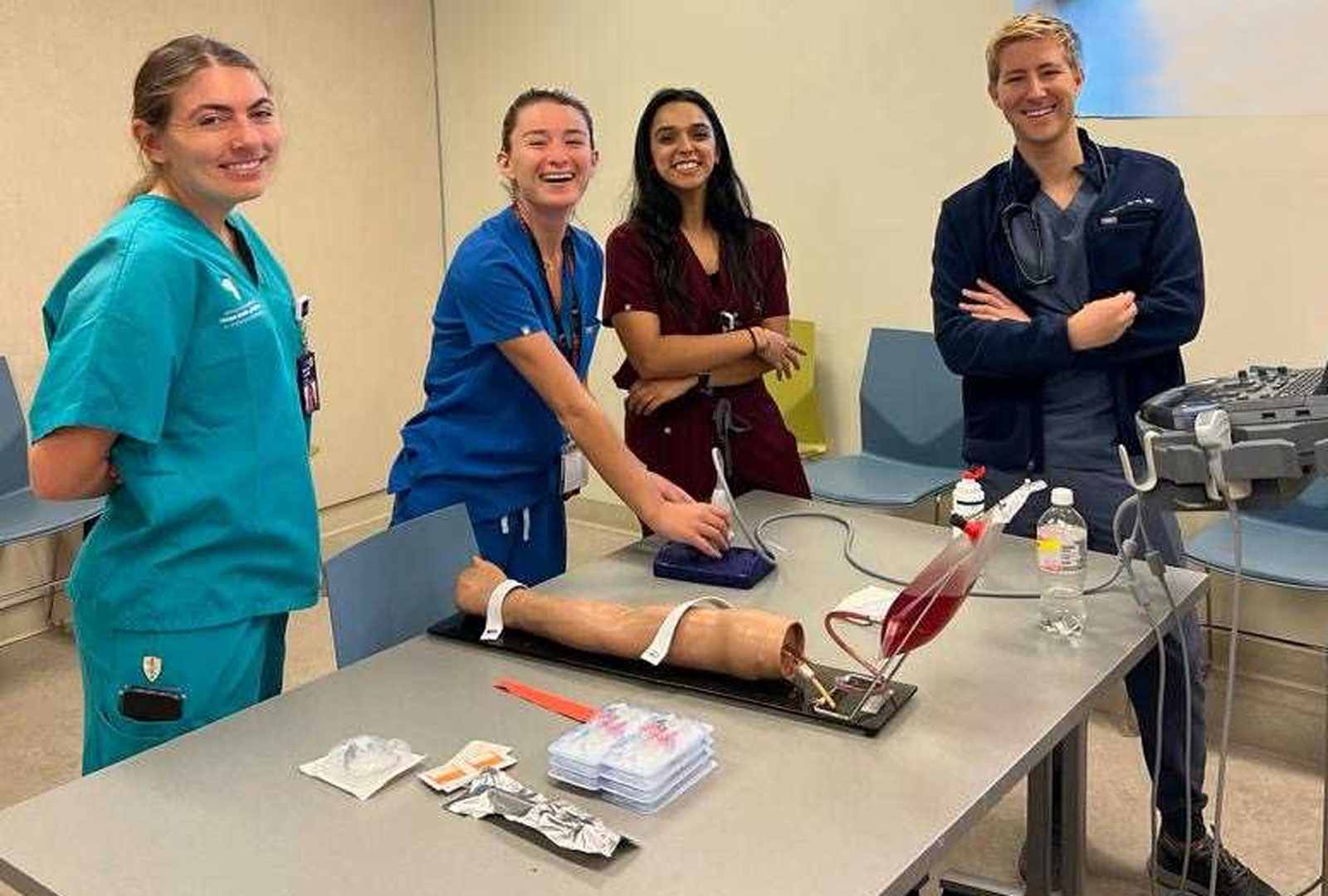
Our one-year preliminary medicine track provides foundational education for residents seeking to complete training in internal medicine or an advanced residency program in a non–internal medicine specialty such as anesthesiology, dermatology, neurology, ophthalmology, radiology, or physical medicine and rehabilitation.
Residents who complete either the categorical medicine residency or the preliminary medicine residency have opportunities to move on to fellowships in a wide variety of specialties.
Program Details
The Internal Medicine Residency program aims include the following:
- provide medical knowledge through patient encounters and didactic sessions to prepare physicians to successfully pass the boards and become competent independent providers who are prepared for unsupervised practice
- provide training to obtain and apply information from patient histories, physical exams, laboratory data, and diagnostic testing to formulate working diagnosis, differential diagnosis, and plans for the evaluation, treatment, and management of medical conditions and comorbidities
- emphasize the interpersonal and communication skills needed to develop patient-centered relationships with patients and families
- enable the progressive development of medical knowledge, including basic science, clinical medicine, epidemiology, and social and behavioral sciences, and apply that knowledge to the care of patients with the goal of lifelong learning
- instill continuous assessment of performance through self-assessment and feedback from supervisors to identify opportunities for improvement
- train physicians to effectively work with the multidisciplinary team and the healthcare system to utilize all available resources to optimize healthcare for patients
- demonstrate commitment to professional responsibility, adherence to ethical principles, and dedication to sensitivity and cultural competency in inpatient care
- provide a support system that allows for personal and professional growth, minimizes burnout, and promotes resilience
The residency program is overseen by Mark J. Corapi, MD, program director, and a complement of associate program directors all dedicated to resident education and success.
Meet our Faculty Leadership APDs
Nicholas Berbari, MD
Shirley M. Hanna, MD
Jonah Feldman, MD
Jamie C. Yedowitz- Freeman, DO
Jonathan S. Shulman, DO
Margaret O’Shea, MD
Robert K. Abdullah, MD
Meet Our Administrative Leadership
Celeste Rachell
Residency Program Coordinator
Robin Coyle
Residency Program Coordinator
Clinical Training
Our Internal Medicine Residency program is a leader and innovator in block model ambulatory education. We offer a 6 + 2 schedule of ambulatory care blocks. This provides an uninterrupted inpatient and outpatient schedule. Residents are assigned to ambulatory clinic multiple times throughout the year.
The dedicated two-week blocks of ambulatory clinic time permits residents to focus, without interruption, solely on outpatient medicine. Each clinic week consists of seeing patients with faculty preceptors and one day of didactic learning dedicated to outpatient topics. Residents learn evidence-based ambulatory medicine, telemedicine, as well as a practical approach to clinical practice, billing and referrals. During the blocks, residents also receive advanced medical interviewing training to optimize their skills in Patient Experience measures. Our residents appreciate their exposure to the way office-based medicine really works. Residents also have opportunities to spend half-days in ambulatory subspecialty clinics of their choice based on their fellowship or career goals.
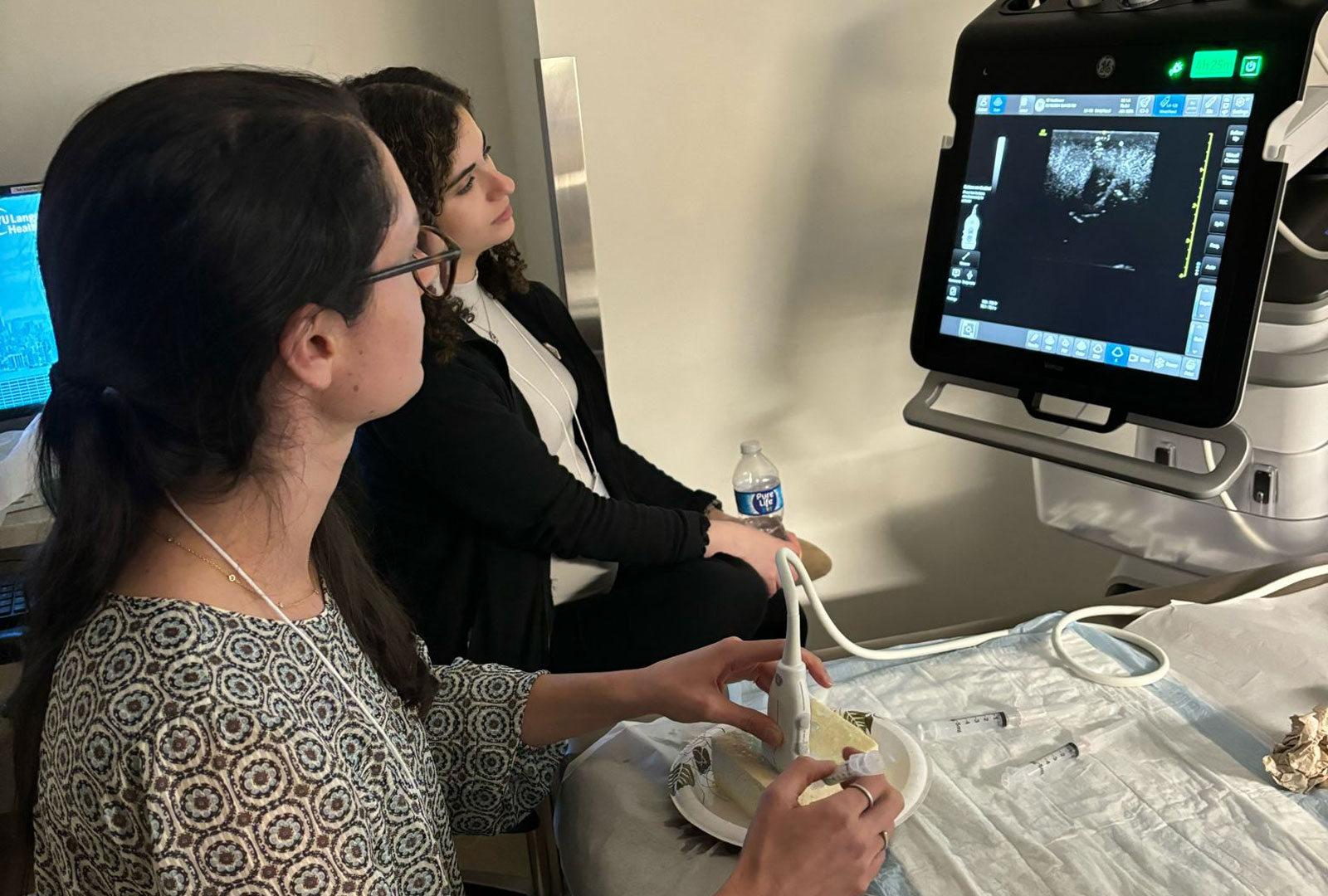
Throughout the three years, residents will rotate on the various wards at the NYU Grossman Long Island School of Medicine hospital. Rotations in our ICU, CCU, oncology, telemetry, and general medicine floors provide comprehensive education. Residents will work as a team under the supervision of an attending where they will learn the foundation of inpatient acute care. Often these educators are awarded attending of the year a testament to their dedication to house staff education and excellent patient care.
Click here for our Rotations Overview
Resident Didactics
The Department of Internal Medicine is committed to providing an expansive didactic learning environment to enhance residents’ clinical experience. The didactic experience includes the following:
- Core Competency lectures and workshops
- Department of Medicine Grand Rounds
- Journal Club
- Afternoon Report Case Conference
- Noon Conference given by core faculty on various topics
- Morbidity, Mortality and Improvement Conference
- Simulation lMb sessions
- Procedural sessions
- Quality Assurance and Improvement
- Board Review
- Joint conferences with other departments
- Weekly full day of didactics during the ambulatory clinic blocks include presentations given by subspecialists on various topics related to non–internal medicine primary care disciplines, including dermatology, ophthalmology, podiatry and otolaryngology.
Electives
With guidance from a faculty mentor, internal medicine residents are encouraged to tailor elective time toward future professional interests and career goals. Elective rotations provide residents with experience in many ambulatory and inpatient subspecialty medicine areas, including anesthesia, cardiology, dermatology, endocrinology, gastroenterology, geriatrics, hematology–oncology, hospitalist medicine, infectious diseases, interventional cardiology, nephrology, neurology, palliative care, perioperative consultation, pulmonary and critical care medicine, radiology, radiation oncology, rheumatology, and sports medicine. Electives are also available in administration and leadership and occupational environmental medicine.
Research Opportunities
The Internal Medicine Residency offers nationally recognized and funded basic science and clinical research opportunities through the many subspecialty divisions in the Department of Medicine, as well as in the other departments. Residents collaborate with co-residents and faculty research mentors in research in the specialty or primary care area of their choice. Resident research has led to publications in peer reviewed journals as well as presentations both locally and at national conferences.
A series of research workshops for residents include topics such as critical appraisal of the literature, statistics, and study design, which residents then apply to their own research projects, as well as during journal clubs, morning reports, and other conferences.

Career Development
Our faculty are committed to helping each resident foster their individual interests to best help them on their journey to becoming the best physician they can be. Our residents have successfully pursued careers in all major subsets of internal medicine. Matching into fellowships of their choosing in our own institution as well as outside institutions. Other residents have continued their love of general internal medicine in both the outpatient primary care setting and inpatient acute care hospitalist field.
Disclaimer: NYU Langone’s programs do not include preferences, quotas, or set asides, or otherwise exclude anyone based on race, sex, or other protected categories.